neuroplex
New York Association of Neuropathologists
4/20/2010 Case 1: PXA with anaplastic features
Presented by: Dr. Jenny Libien - Kings County Hospital
Clinical History:
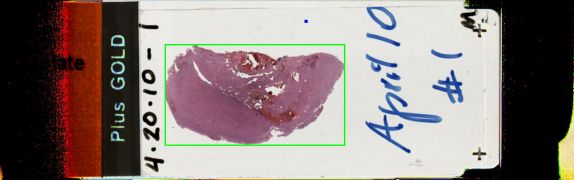
The patient is a 41 year old Nigerian woman (G5P4004) who came to the United States one month prior to presentation. She was 35 weeks pregnant, recently diagnosed with gestational diabetes, and she complained of headache during a prenatal appointment. The headache was on the right side, behind her eye and pulsating. The pain had been severe and intractable for the two months prior to presentation but had been present for approximately 3 years. The patient was sent to the Emergency Department. MRI showed a large extra-axial mass with an internal hemorrhagic component and extensive surrounding vasogenic edema in the right frontal lobe. There was compression of the right frontal horn of the right lateral ventricle. Neurologic exam was significant for blurred optic discs. The patient was admitted, and a healthy infant was delivered via C-section. One week later, a total resection of the right frontal mass was performed by Neurosurgery. A 4.5 a 4 x 3.5 cm mass was received by Pathology. On sectioning, the mass had a variegated appearance, with multifocal areas of hemorrhage, a central soft area, and firm whitish regions.
Sections showed a pseudoencapsulated, infiltrating tumor with large eosinophilic cells with copious glassy to vacuolated cells with a perivascular pattern. Nuclei were eccentric with prominent nucleoli, and some were multinucleated. There were mitoses, hemorrhage and pseudopalisaded necrosis. The tumor contained GFAP-positive cells with processes and was reticulin poor. CD34 was positive in a membrane pattern. The tumor expressed S100, synaptophysin and vimentin. It was negative for NeuN, CAM5.2, EMA, p53, HMB45 and neurofilaments. The MIB1/KI67 was variable from 1-10%. The differential diagnosis included giant cell glioblastoma, pleomorphic xanthoastrocytoma (PXA), anaplastic ependymoma and astroblastoma.
Diagnostic Notes:
Dr. Libien's diagnosis was PXA with anaplastic features, WHO Grade III. Discussion centered on the differential diagnosis. Dr. Rosenblum agreed that the tumor was Grade III but suggested that CD99 might be positive and wondered if the tumor could represent an anaplastic ependymoma because that entity may show membraneous CD34 staining and the negative EMA is not helpful. In addition, PXA may be reticulin-poor. He suggested that electron microscopy might be helpful. One could call this tumor "anaplastic glioma" and not go any further.
This neoplasm has not recurred six months after surgery.
References:
- Frank S, Cordier D, Tolnay M, Rosenblum MK. A 28 year old man with headache, visual and asphasic speech disturbances. Brain Pathology 2009;19:163-166.
- Asano K et al. A case of anaplastic pleomorphic xanthoastrocytoma presenting with tumor bleeding and cerebrospinal fluid dissemination. Brain Tumor Pathology 2006;23:55-63.
- Primavera J et al. Clear cell pleomorphic xanthoastrocytoma: case report. Acta Neuropathol 2001;102:404-408.
- Reifenberger G, Kaulich K, Wiesteler OD, Blumcke I. Expression of the CD34 antigen in pleomorphic xanthoastrocytomas. Acta Neuropathol 2003;105:358-64.